Recovering from a brain injury can be a long process. Patients go through various stages of rehabilitation and recovery. Patients who can transition through each stage increase the likelihood of healing, aiming to move the patient as close as possible to their pre-injury condition.

Generally, there may be ten stages that a patient with a traumatic brain injury (TBI) may experience or progress through. However, not every person will experience each stage in identical ways, and each survivor will recover at a different pace.
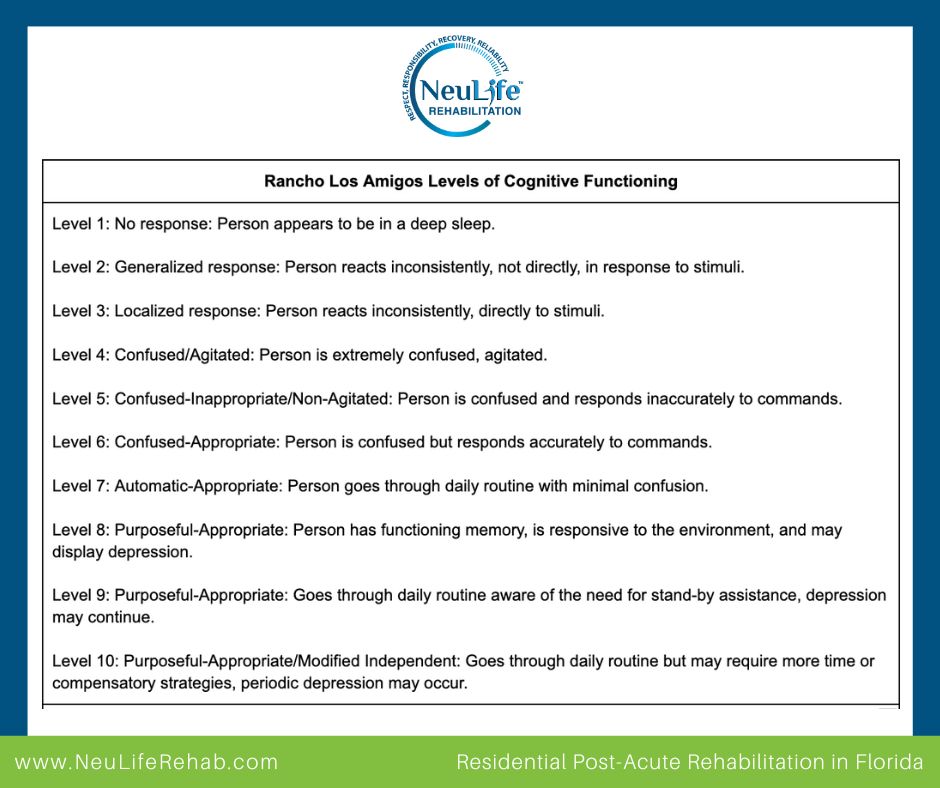
This blog post will walk you through the 10 stages of TBI recovery based on the Rancho Los Amigos Levels of Cognitive Functioning and highlight techniques to promote optimal healing.
The Rancho Los Amigos Scale was developed at the Rancho Los Amigos National Rehabilitation Center in California. It is a widely used clinical tool that describes the cognitive and behavioral patterns of TBI patients during recovery.
The scale consists of 10 levels, ranging from complete unresponsiveness to the ability to function independently. Understanding these stages helps medical professionals, caregivers, and families set realistic expectations and provide appropriate support.
A coma is the deepest state of unconsciousness. It allows the brain to heal uninterrupted. With a severe injury, the patient may remain in a coma for some time. This is considered the first stage of TBI recovery.
What to expect:
Generally, coma patients have no eye movement, no purposeful movement, and lack speech and communication. The patient is unresponsive to the environment and does not wake, even with stimulation.
Comas can last weeks, months, or even years. After awakening from a coma, the patient may move through further stages of recovery.
Care approach:
Comas and a vegetative state are not the same; they are different states of consciousness. Neurological responses differ between these two. Patients in a coma have no neurological response, while those in a vegetative state may have regained some reflexes.
What to expect:
In a vegetative state, the patient may appear awake. You may see eye movement, reaction to stimulation, and involuntary body movements. These movements are caused by responses in the brain that remain intact after injury and because areas of the brain have begun to heal.
Care approach:
Once patients react and can communicate, they move to the next stage of recovery.
During this stage, patients may come in and out of consciousness. The significant improvement seen is awareness of people and surroundings. When in this stage, medications can help stimulate the brain to regain consciousness.
What to expect:
The patient responds more deliberately to specific stimuli, such as turning their head toward a voice or following simple commands. They begin to recognize familiar faces and have more purposeful movements.
Care approach:
As the patient responds to instructions and communication, they move toward recovery.
Post-traumatic amnesia is the stage after the patient emerges from a coma. They may experience a state of amnesia upon awakening. There are two types of amnesia:
What to expect:
Some patients may show behavior changes in this stage. They may become highly confused and aggressive or show other signs of inappropriate behavior. Patients can also lose their sense of inhibition, especially if the frontal lobe experiences an injury.
They may also experience difficulties processing information and not recognizing their surroundings.
Care approach:
Once patients can consistently remember daily events and amnesia diminishes, they are usually ready to begin rehabilitation at a neuro rehab facility, where true healing and recovery begin.
In this stage, patients can have difficulty focusing on tasks and may be confused. It can be challenging for them to respond during communication or express inaccurate or unintelligible communication.
What to expect:
During this stage, their short-term memory is still impaired, so expect them to experience difficulties in communication and learning new information. They may also do random speech with little awareness of conversation.
Care approach:
If you want to learn more about inappropriate behavior after TBI, check out our blog post on brain injury and inappropriate behavior.
During this stage, the patient may be able to communicate and follow more commands from staff. However, memory issues often still exist, and focusing on tasks can be challenging.
What to expect:
Expect patients to have better attention spans but still be forgetful. With help, they can now engage in familiar activities.
Care approach:
When patients advance to this stage in their recovery, they can begin to follow a schedule and complete some daily life activities independently.
This is an essential stage in post-acute rehabilitation, as patients can participate in important rehab recovery efforts, including physical therapy, occupational therapy, and speech therapy.
What to expect:
Patients may have improved memory for familiar tasks but struggle with problem-solving, decision-making, and planning skills.
Care approach:
At this stage, the patient's awareness and memory have improved. However, the patient may continue to struggle with social interaction, reaction time, and handling unexpected situations that are not part of their routine.
That said, they often have made significant improvements in their coping skills and may sometimes be able to graduate from a rehabilitation facility and return home.
Care approach:
The TBI patient has gained function in this stage and can perform most tasks independently. They likely will need to have continued rehabilitation for brain injury but do not require the full assistance of a neurorehabilitation center.
What to expect:
Patients in this stage can manage appropriate activities independently but may need assistance in complex or unfamiliar situations. Furthermore, they have improved emotional stability and can make decisions with occasional support.
Care approach:
During this final stage, some patients have a full recovery and can handle daily life activities on their own. However, their cognition may remain slower than pre-injury, which they usually do well with, and they can participate in outpatient neuro services if necessary.
Care approach:
Maximizing recovery potential requires a combination of medical, cognitive, and emotional support. Here are some key techniques:
Neulife Rehab is one of Florida's most extensive brain injury facilities in the southwest United States. Neulife is CARF-accredited (Commission on the Accreditation of Rehabilitation Facilities) in Brain Injury Specialty Programs and Residential Rehabilitation.

Through rehabilitation, medical management, psychiatric, neurophysical services, occupational, speech, and cognitive therapies, and much more. We provide different types of programs, from traumatic brain injury rehabilitation to stroke patient rehab. We provide the best in care so your loved one has the BEST POSSIBLE recovery.
Schedule a tour to see our facility and decide if it may be appropriate for your loved one. We are always here to answer questions. Please reach out to us at 1-888-626-3876.
The material contained on this site is for informational purposes only and DOES NOT CONSTITUTE THE PROVIDING OF MEDICAL ADVICE, and is not intended to be a substitute for independent professional medical judgment, advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare providers with any questions or concerns you may have regarding your health.

We know that choosing the next step in your recovery from a catastrophic illness or injury is complex. Together, we can help you take the next step.
Contact us with any questions today.